
for mothers
Below we have collected relevant information about perineal tears, what they are, their impact on women, and common prevention techniques today.
This content on this page is provided for general information and awareness only and does not constitute medical advice. It does not replace clinical judgement. Mothers should consult their midwife, obstetrician or other healthcare professional for advice specific to their situation.
What are perineal tears and how do they affect women today?
Perineal tears are the most common complication of vaginal childbirth. They are tearing of skin, tissue, but most importantly, in most cases also muscles. These tears can impact you after birth in many different ways The more severe the tear, the more likely of severe consequenses. However, tear 2 can also lead to long term consequenses impacting quality of life.
-
Immediate surgical repair: Tears during childbirth often need to be stitched. This can cause unexpected pain and stress for the mother. Many women feel they were not fully prepared for this, and even small tears can take up to an hour to repair.
Postpartum bleeding: Tears can increase the risk of heavy bleeding after birth. This may require urgent treatment and can make recovery longer and more difficult.
-
Ongoing pain after birth: Pain in the perineal area can last for several weeks or even months after childbirth. More severe tears can cause stronger and more constant discomfort, making it difficult to sit, walk, or comfortably hold the baby.
Dependence on pain relief: Many women need pain medication after experiencing tears. This can slow down recovery and make everyday activities more challenging.
Emotional impact: Perineal tears can also affect emotional wellbeing. Some women experience stress, anxiety, or feelings of trauma, which can overshadow what is often expected to be a joyful time.
Impact on breatfeeding and bonding: Pain and stress from tears can make it harder to start breastfeeding. This, along with physical discomfort, may affect early bonding between mother and baby.
-
Sexual health: Some women experience pain during or after sex following childbirth tears. This can last for months or years and may affect intimacy and relationships.
Urinary incontinence: Tears that affect the muscles can lead to difficulty controlling urine. This may impact daily life, including exercise, work, and social activities.
Anal incontinence: Third- and fourth-degree tears can damage the anal sphincter, leaving some women unable to fully control bowel movements— one of the most stigmatizing and isolating consequences of perineal trauma.
Pelvic floor dysfunction: Tearing can weaken the pelvic floor muscles, leading to feelings of heaviness, discomfort, or difficulty with muscle control.
Pelvic organ prolapse: Damage to the pelvic floor can increase the risk of organs shifting from their normal position. This can cause discomfort and make everyday activities like moving, exercising, or working more difficult.
Mental health impacts: Severe tears can increase the risk of anxiety, depression, and post-traumatic stress. This can affect both the early experience of parenthood and long-term wellbeing.

Who is at risk of perineal tears?
In short all women is at risk. 85 % of all women suffer from perineal tears during vaginal birth. There are certain things which increase the risk of tears according to the clinical litterature, however, it does not automatically lead to tearing.
-
Long labor and pushing: A long pushing phase or extended labor can put extra stress on the tissues, increasing the chance of tearing.
Instrumental births: Births that involve tools such as a vacuum or forceps carry a higher risk of tearing, especially for first-time mothers.
Episiotomy: An episiotomy is a cut made to help deliver the baby. While it may sometimes reduce the risk of more severe tears, it still results in a tear and its benefits are debated.
Rapid births: When a baby is born very quickly, the tissues may not have enough time to stretch gradually, which can increase the risk of tearing.
Epidural and assisted delivery: Epidurals are not directly linked to more tearing, but they can increase the likelihood of needing an assisted birth, which raises the risk.
Vaginal birth after C-section (VBAC): Women who have a vaginal birth after a previous C-section may have a higher risk of tearing.
-
First-time birth: Women giving birth for the first time have a higher risk of experiencing tears.
Previous severe tear: If a woman has had a severe tear in a previous birth, there is a higher chance it can happen again in a future vaginal birth.
Short perineal length: A shorter distance between the vaginal opening and the anus (perineal body) is linked to a higher risk of more severe tears.
-
Larger baby size: Babies with a higher birth weight or larger head size can increase the likelihood of tearing during birth.
Baby’s position during birth: If the baby is in a less optimal position (such as facing upwards) or if the shoulders become stuck during delivery, this can put extra strain on the perineum and increase the risk of tearing.
How are perineal tears prevented today,
and what does clinical evidence say?
-
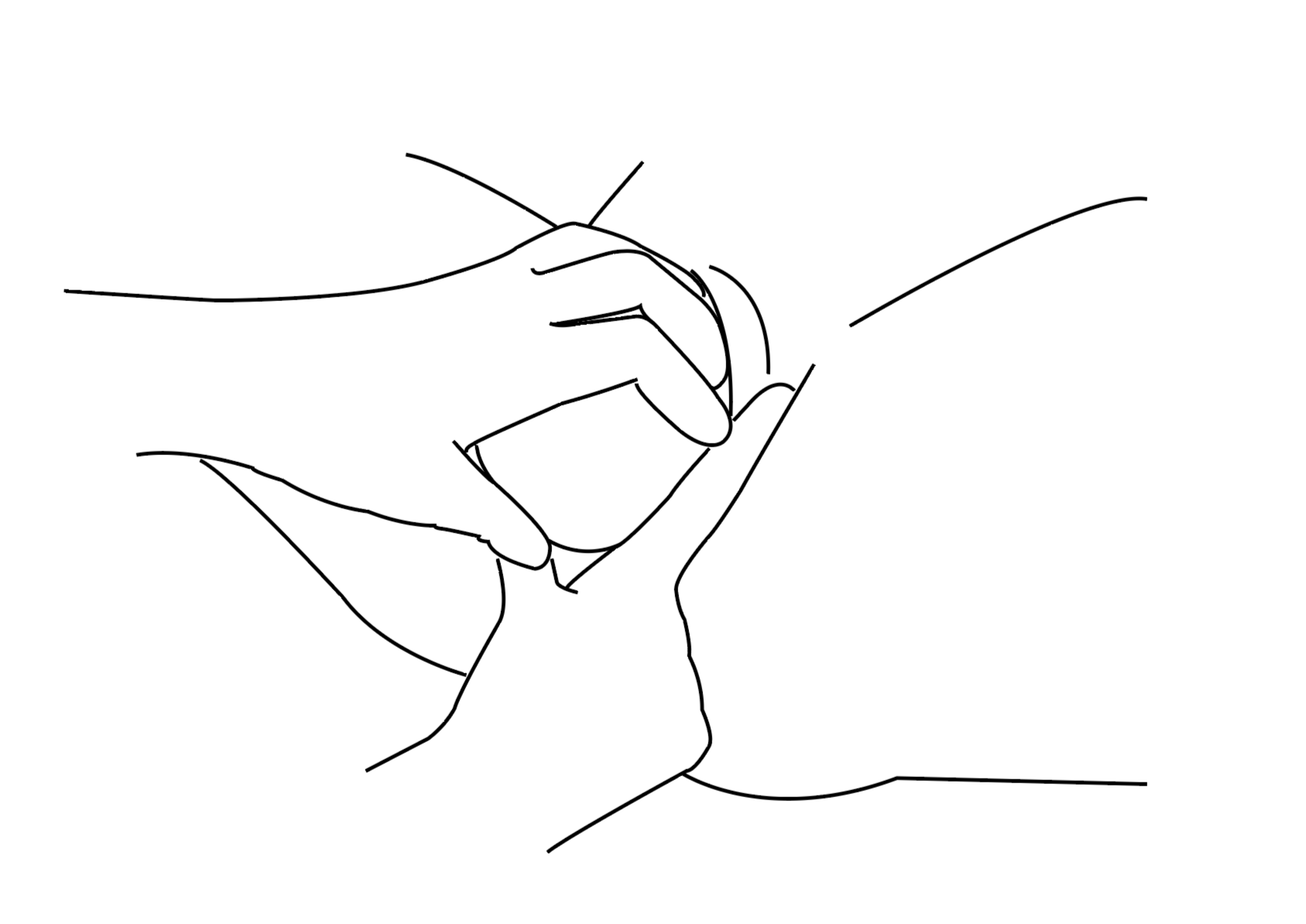
Manual perineal protection
Midwives are trained to use their hands to support the perineum during the pushing stage of labor. When applied consistently and correctly, this technique is associated with reduced risk of severe tears. However, both the use of this approach and how it is performed can vary between hospitals and regions.
-
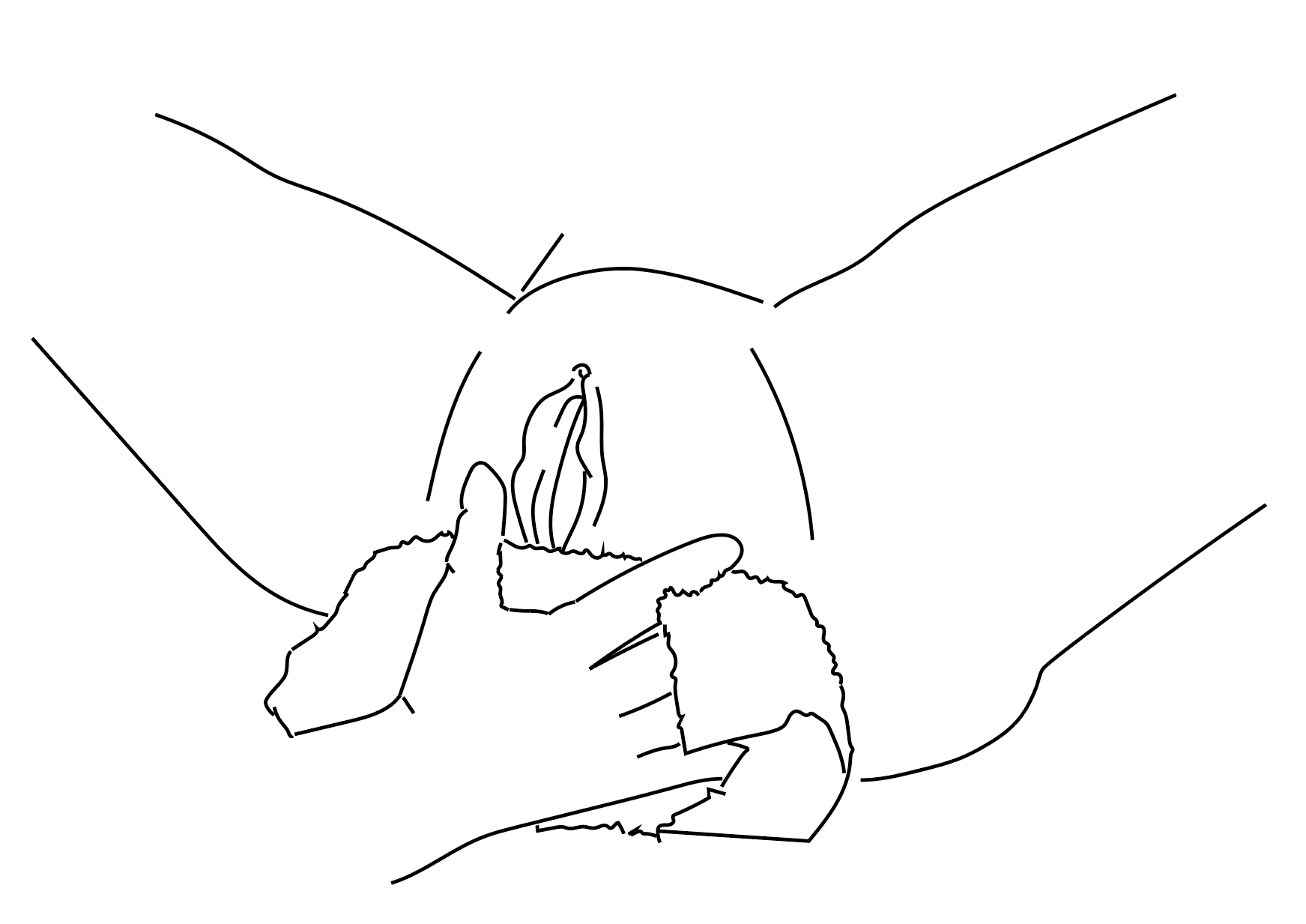
Warm compresses
Warm compresses or gentle pressure may be applied to the perineum during labor to improve comfort and support tissue stretching. Some evidence suggests these methods may help reduce tearing, but the overall evidence remains limited. In practice, their use is inconsistent and not standardized across hospitals.
-
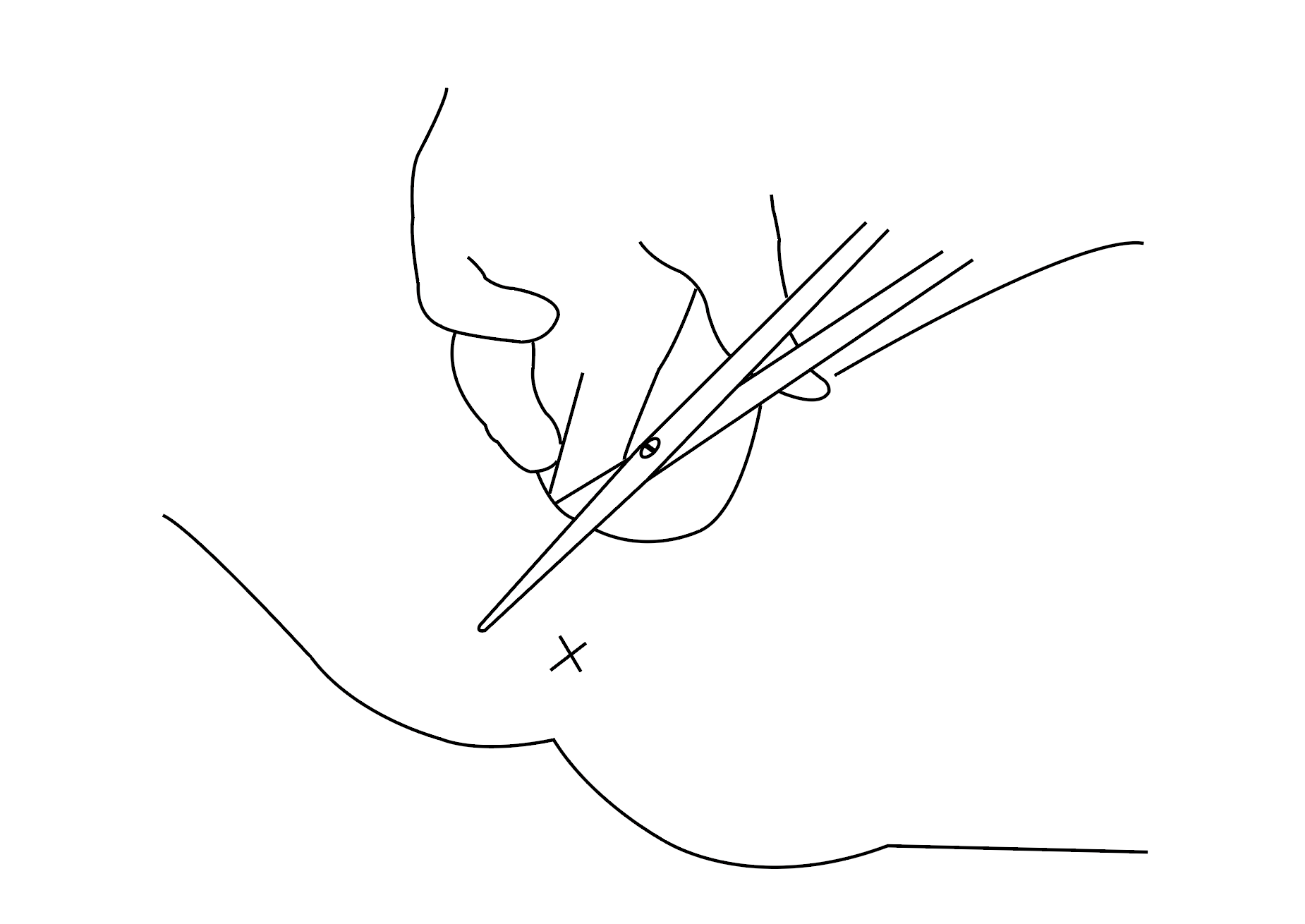
Episiotomy
A mediolateral episiotomy may be performed in certain situations, most often during instrumental births, to help reduce the risk of severe tearing. Routine use is not recommended. While it can be beneficial in specific cases according to evidence, unnecessary use may lead to slower healing and increased postpartum pain.

What does current research say about actions women themselves can take to prevent tears?
Research on preventing perineal tears is still evolving, and strong evidence is limited. However, some aspects related to a woman’s own preparation and choices during pregnancy and labour have been studied, particularly among first-time mothers.
Antenatal perineal massage
Antenatal perineal massage is a technique that can be performed by the woman herself in the final weeks of pregnancy, typically from around week 34. It involves gently stretching the tissue around the vaginal opening using fingers or thumbs.
Some studies suggest that this practice may be associated with a reduced likelihood of perineal trauma requiring suturing and a lower rate of episiotomy, particularly in first-time vaginal births. It has also been linked in some research to reduced perineal pain after childbirth. However, findings across studies vary, and the overall level of evidence remains limited.
Birth position during labour
A woman’s choice of position during labour and birth has been explored in relation to perineal outcomes. Upright positions — such as kneeling, squatting, or sitting — have been associated with lower rates of episiotomy and instrumental birth compared with lying on the back. Instrumental births (forceps or vacuum) are linked with a higher risk of severe perineal tears.
There is no single position that has been shown to prevent tearing. However, being able to move freely and change positions during labour is commonly described in clinical literature as part of supporting a physiological birth process.
While several techniques are used and researched today to prevent perineal tears, there is still limited consistency in how perineal support is applied during childbirth. Perineal protection devices are gaining interest as a potential perineal protection strategy and are developing a growing body of evidence.
At oasicare we have developed ASISU™ to support innovation in perineal care in this new emerging field.

What is ASISU™?
ASISU™ is a perineal protection device designed to be used during birth by your midwife or health care professional. The device is designed to distribute the forces on your perineal tissue, to help reduce stress peaks that cause perineal tearing.
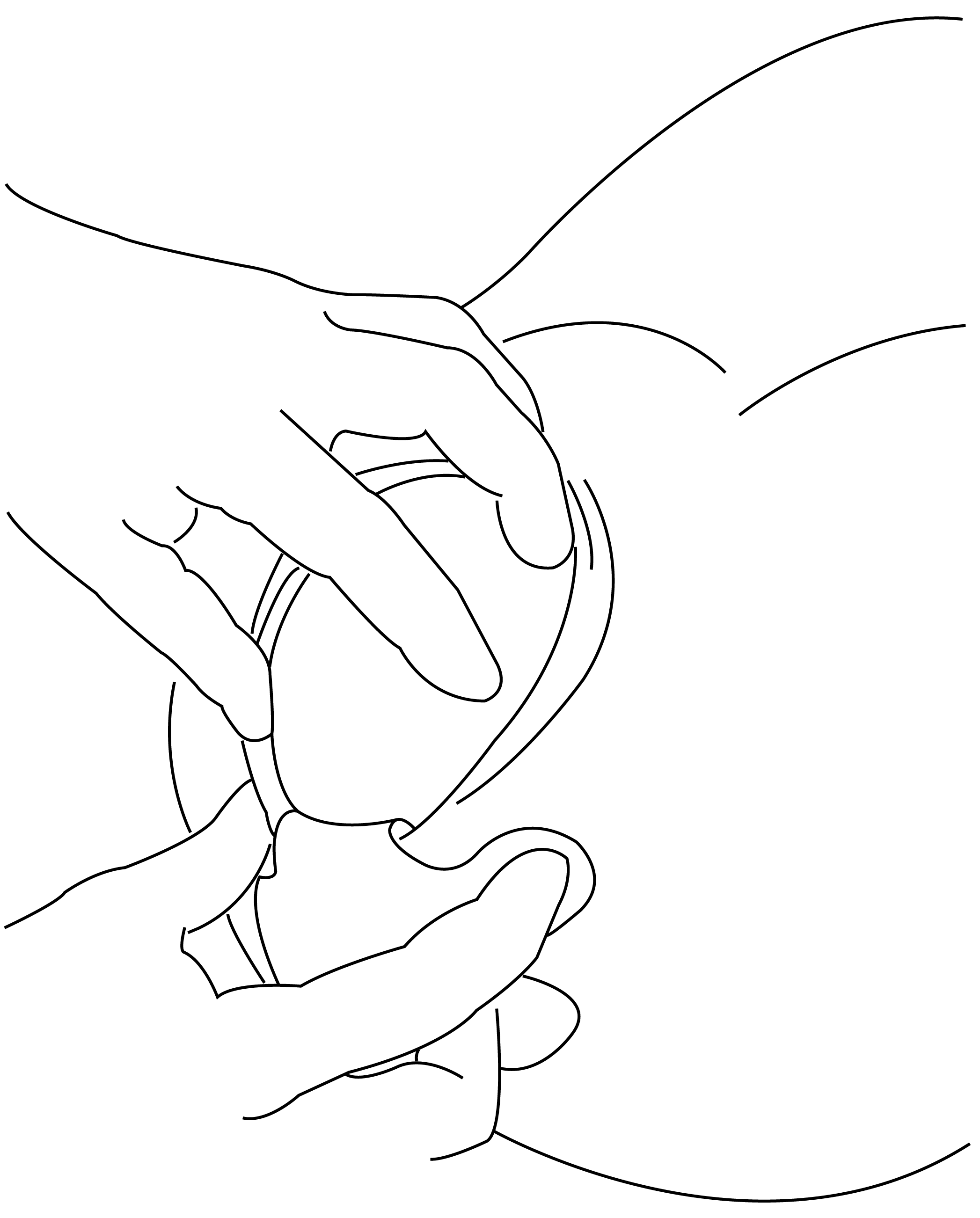
For full instructions, warnings, contraindications and residual risks, see the IFU.
Because women deserve better
You may have heard that research into women-specific conditions receives only a small share of overall funding — around 1%. For decades, women’s health has received less investment than other areas of medicine. Much of medical research has historically been based on male biology, leaving critical gaps in our understanding of women’s health —especially in pregnancy, birth and maternal care.
For us at oasicare it is clear that childbirth should not come at the cost of a woman’s long-term quality of life. Mothers deserve better, and we are here to challenge the status quo through innovation.

“Simply surviving pregnancy and childbirth can never be the marker of successful maternal healthcare.”
World Health Organization (WHO)
Would you like to share your story with us?
With perineal tears or maybe experiences related to birth with our device? Or maybe interested in participating in the development of ASISU?
Oasicare is deeply committed to developing women-centered innovation. We want to continuously involve women — listening to their experiences, gathering feedback, and understanding what perineal tears truly mean in real life, both for those of you preparing to give birth and those of you who have already gone through it. Get in touch below.

